Simulation 3. Oral Health Risk Assessment
IOH ToolkitChapter 5. Simulation Learning
Simulation 3. Oral Health Risk Assessment
Authors: Pooja Bhalla, MSN, RN, Adjunct Faculty, School of Nursing, Bouvé College of Health Sciences, Northeastern University and Colleen Anderson, DDS, Associate Dental Director, Boston Health Care for the Homeless Program.
At-a-Glance
| Topic | Oral health risk assessment |
| Academic Focus | Clinical skills |
| Target IPEC Competencies | Domain: Roles and Responsibilities
Engage diverse healthcare professionals who complement one’s own professional expertise, as well as associated resources, to develop strategies to meet specific patient care needs. |
| Target HRSA Competencies | Domain: Risk Assessment
Conduct patient-specific, oral health risk assessments on all patients. Domain: Communication and Education Provide targeted patient education about importance of oral health and how to maintain good oral health, which considers oral health literacy, nutrition, and patient’s perceived oral health barriers. |
| Learning Objectives | Describe the impact of oral health on systemic health and chronic disease management. Identify risk factors that impact oral health. Identify and describe the impact of risky behaviors on oral health. |
Instructor’s Guide
Background. This simulation was pilot tested with a group of case managers, medical assistants, and respite aides in a patient-centered medical home (a primary care practice that has adopted a set of practices aimed at coordinating and improving the delivery of patient care). This simulation can be adapted for use with students of any health profession.
Overview for instructors. The purpose of this exercise is to provide health professions students the opportunity to interview a patient, make an oral health risk assessment, and determine the need for referral. This simulation does not incorporate an oral examination as part of the risk assessment. It can be performed in any type of environment necessary (i.e., clinic, bedside, doctor’s office, or classroom).
Materials provided in this toolkit.
- Case Scenario 1 and Case Scenario 2 with complete information for instructors and for actors portraying patients.
- Handouts for students:
Additional materials.
- None
Instructor preparation.
- Recruit one or two trained actors to play the role of patient. The number of actors you recruit will depend on how many students you are training.
- Review the patient case scenarios with the standardized patients.
- Practice the simulation with the standardized patients prior to the actual simulation.
- Assign students to groups of five or six and create a simulation schedule that allows 30 minutes for each group to complete the exercise. It may be helpful to send students their group assignments and simulation schedules prior to the simulation.
Student preparation.
- Students should register for and complete the following Smiles for Life courses.
- Course 1: The Relationship of Oral-Systemic Health
- Course 3: Adult Oral Health
- Students should review the ADA Caries Risk Assessment Form (Age>6) contained in this toolkit.
Schedule.
- Simulation orientation (5 minutes)
- Simulation (15 minutes)
- Debrief (10 minutes)
Instructor’s Notes
This simulation will take approximately 30 minutes for each group of students to complete.
Simulation orientation (5 minutes). Review learning objectives.
- Describe the impact of oral health on systemic health and chronic disease management.
- Identify risk factors that impact oral health.
- Identify and describe the impact of alcohol use, tobacco use, or other risky behaviors on oral health.
Review the simulation process with the students.
- State the length of the simulation (30 minutes).
- Review the ADA Caries Risk Assessment Form Age >6 and the Dental Referral Form.
- Explain that one student in each group will act as the provider and all other students in the group will act as observers.
- Emphasize that only the provider will interact with the patient while all other students observe.
Simulation (15 minutes).
- Role of provider. The provider in each group will interact with the patient by reading from a script while the other students observe. After the standardized patient presents with findings outlined in his or her patient case scenario, the provider will:
- View a photograph of the presenting clinical condition the patient described.
- Complete the ADA Caries Risk Assessment Form Age >6.
- Offer the patient anticipatory guidance based on the clinical findings in the photograph.
- Make a dental referral using the Dental Referral Form if necessary.
The provider should refer to the Critical Items Checklist for Simulation 3 throughout the clinical encounter.
- Role of student observers. The observers should watch the provider interact with the patient and read along with the script as the interview progresses. Observers should make independent decisions regarding assessment, recommendations, and referral while filling out their own copies of the ADA Caries Risk Assessment and the Dental Referral Forms. Observers should not communicate during the simulation.
The observers should refer to the Critical Items Checklist throughout the clinical encounter.
Debrief (10 minutes). Generate open discussion about the simulation by inviting reactions from both the standardized patient and the students. To prompt discussion, ask students to consider the given patient history and specific clinical findings. Then ask debriefing questions.
- How did you classify the patient’s risk status (low, moderate, high)?
- What specific recommendations did you have for this patient?
- What did you think of the anticipatory guidance the provider offered the patient? Would you have offered anything different?
- Would you refer the patient to a dental provider? If so, why?
Case Scenario 1 (Instructor/Actor Copy)
Patient information.
Name: Veronica
Age: 45
Setting: Medical triage
Chief concern: Patient wants to discuss her diabetes. Her blood sugar levels have been high.
Medical History:
- Type 2 diabetes mellitus
- History of alcohol abuse but not currently using
- High blood pressure
- No other general health conditions
Script. As part of her appointment, you decide to address the patient’s oral health.
Provider: Do you see a dentist?
Patient: I don’t right now.
Provider: Do you drink tap water or bottled water?
Patient: I don’t drink much water, but if I do it’s through the tap.
Provider: Do you use toothpaste with fluoride in it?
Patient: I guess. I just buy what’s on sale at the store, and I try to brush everyday. Sometimes I forget. I don’t floss because it makes my gums bleed.
Provider: How often do you eat or drink sugary foods?
Patient: I drink coffee throughout the day with regular sugar. Sugary foods once in a while.
Provider: Do you have any mouth pain?
Patient: Sometimes. My gums get sore, and I bleed when I brush.
Provider: How intense and frequent is the pain?
Patient: It’s not sharp, it feels like throbbing, every time after I brush.
Provider: Do you wear dentures?
Patient: No. I don’t have any teeth missing.
Provider: Do you experience dry mouth?
Patient: Not that I’m aware of.
Provider: Do you smoke or use tobacco products?
Patient: Yes. I smoke cigarettes.
Provider: How many a day?
Patient: About half a pack.
Provider: Are you interested in cutting down or quitting?
Patient: No. Not now.
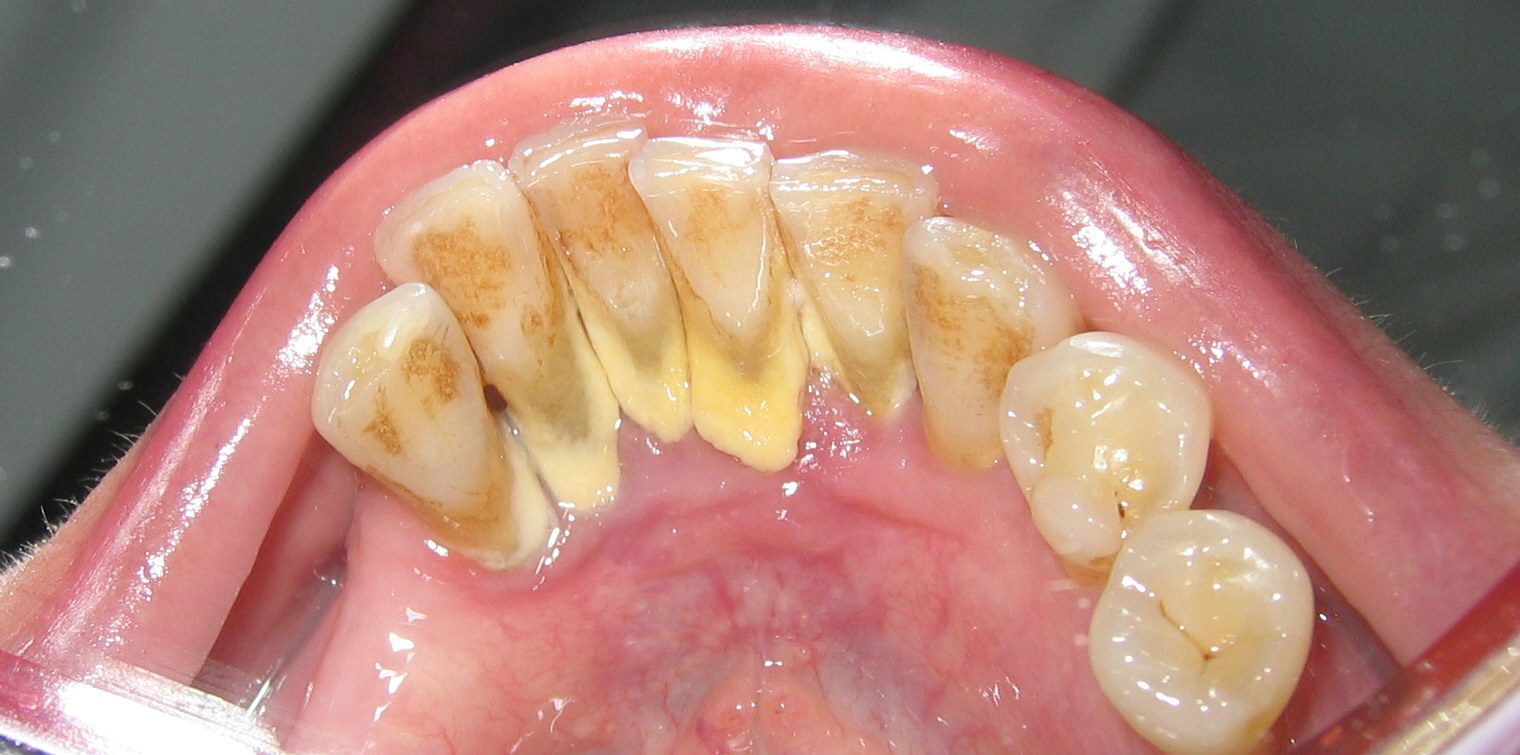
Photo: public domain
- Summary. The presence of diabetes places Veronica at a high risk for gum disease. Her history of alcohol abuse and current smoking habit also place her at an automatic high risk for tooth decay and oral cancer. Further contributing to her risk of tooth decay is her lack of proper oral hygiene and consumption of coffee with sugar throughout the day. The photograph reveals heavy plaque buildup and inflamed gums.
- ADA Caries Risk Assessment. Veronica is at moderate to high risk for caries due to little fluoride exposure, exposure to sugary drinks throughout the day, lack of a dental home, and visible plaque. These findings demonstrate that the provider does not need to address every category of the ADA Caries Risk Assessment to determine the patient needs a dental referral.
- Patient specific recommendations. Refer Veronica to a dental provider for a comprehensive evaluation. Recommend she drink more water throughout the day, use toothpaste with fluoride while brushing twice a day, floss everyday, replace the sugar in her coffee with an artificial sweetener, and smoke less. Educate Veronica on the connection between diabetes and gum disease. If she is interested, provide Veronica with information about services that might help her quit smoking.
Case Scenario 2 (Instructor/Actor Copy)
Patient information.
Name: Vance
Age: 57
Setting: Primary care clinic
Chief concern: Follow-up visit after receiving new medications for high blood pressure and depression
Medical history:
- High blood pressure (taking medication)
- Depression (taking medication)
- No other general health conditions
Script. As part of Vance’s appointment, you decide to address his oral health.
Provider: When was the last time you visited a dentist?
Patient: I had dentures made about a year ago to replace some teeth that got pulled, and I haven’t been since because the office is far and hard to get to.
Provider: How are your dentures fitting?
Patient: Pretty good, but sometimes I have trouble eating because they rub against my gums.
Provider: Do you take your dentures out at night?
Patient: Yes, because my mouth is really dry and it feels good to my gums when I take out my dentures.
Provider: How often do you get dry mouth, and what do you do about it?
Patient: Pretty often since I started the medications. To help I’ll drink something refreshing like lemonade or a sprite.
Provider: How often do you drink lemonade or sprite?
Patient: I like to sip on it during the day while I work or watch television.
Provider: How many times a day do you brush and floss?
Patient: I brush twice a day, I floss every once in a while. I try to be better about it.
Provider: Do you smoke or use tobacco products?
Patient: Yes, I smoke.
Provider: How often?
Patient: About seven or eight a day.
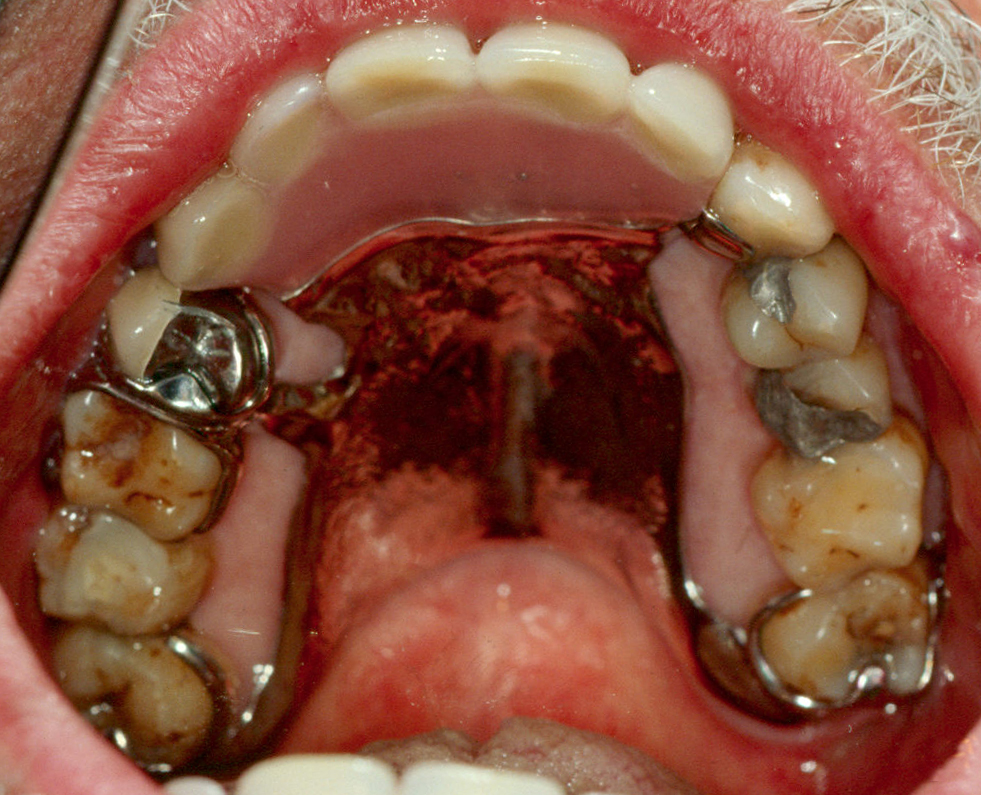
Photo: public domain
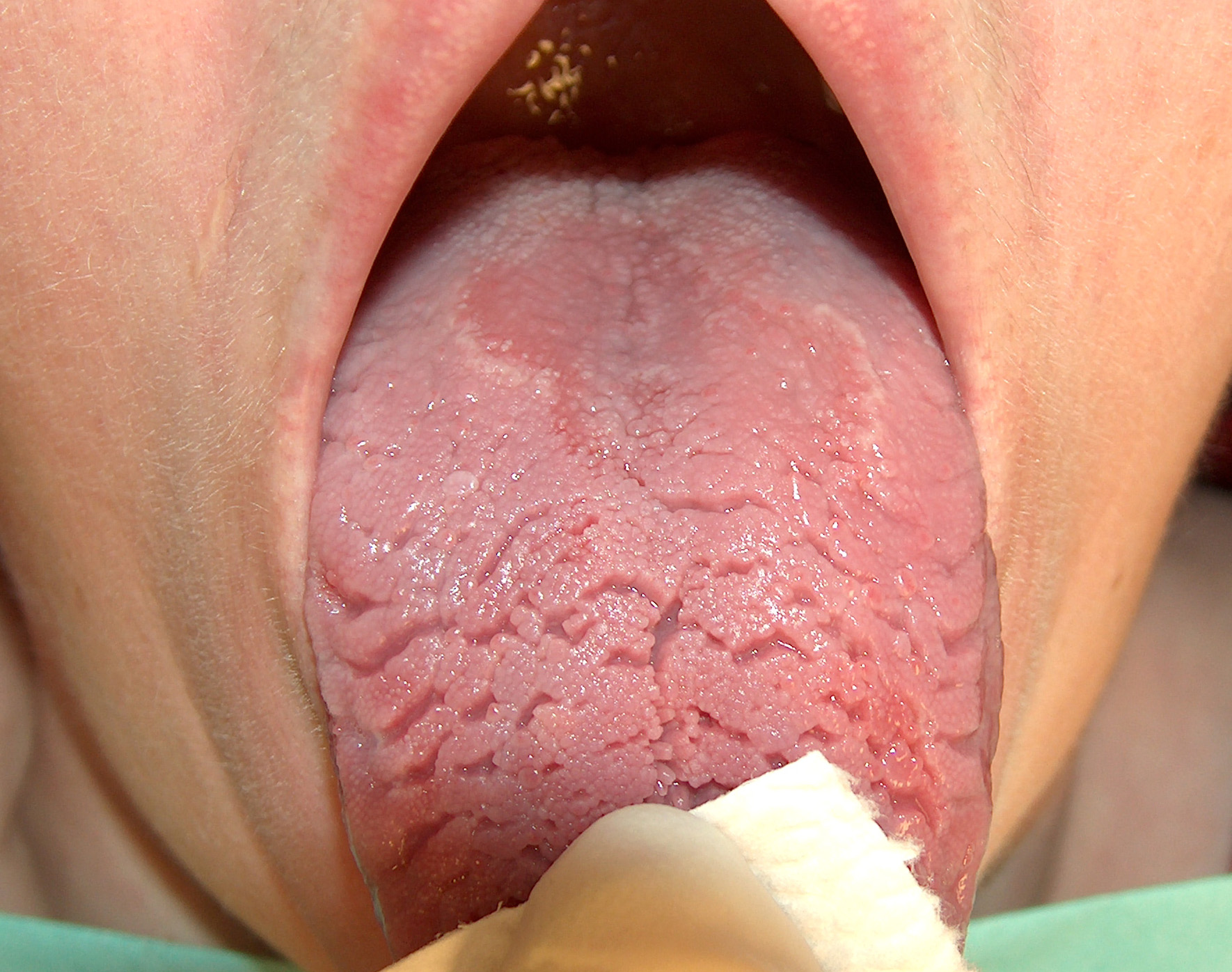
- Summary. The fact that Vance has removable dentures to replace pulled teeth indicates a history of oral disease and places him at high risk for dental caries (tooth decay). His medications are causing dry mouth, which is a common side effect. This also places him at an increased risk for dental caries. The patient’s consumption of sugary drinks and use of cigarettes only worsens his dry mouth and further increases his risk of decay. The photograph shows very dry mouth and fissured tongue.
- ADA Caries Risk Assessment. Vance is at high risk for caries due to exposure to sugary drinks throughout the day, lack of a regular dental home, and a recent history of tooth decay. These findings demonstrate the provider does not need to address every category of the ADA Caries Risk Assessment to determine the patient needs a dental referral.
- Patient specific recommendations. Refer Vance to a dental provider for a comprehensive examination and consultation regarding his dentures, the consequences of dry mouth (caries), and information about how to prevent dry mouth. Recommend flossing and a fluoride rinse. If he is interested, provide Vance with information about services that might help him quit smoking.
First Published: 11/2015
Last updated: 03/2016


