Simulation 2. Oral Conditions and Speech
IOH ToolkitChapter 5. Simulation Learning
Simulation 2. Oral Conditions and Speech
Author: Emily Zimmerman, PhD, CCC-SLP, Assistant Professor, Department of Communication Sciences and Disorders, Bouvé College of Heath Sciences, Northeastern University.
At-a-Glance
| Topic | Oral conditions and speech |
| Academic Focus | Clinical skills |
| Target IPEC Competencies | Domain: Roles and Responsibilities
Engage diverse healthcare professionals who complement one’s own professional expertise, as well as associated resources, to develop strategies to meet specific patient care needs. |
| Target HRSA Competencies | Domain: Oral Health Evaluation
Identify and prioritize strategies to prevent or mitigate risk for oral and systemic diseases. Domain: Interprofessional Collaborative Practice Apply interprofessional practice principles that lead to safe, timely, efficient, effective, equitable planning and delivery of patient and population-centered oral health care. |
| Learning Objectives | Promote an in-depth understanding of how dentistry and speech-language pathology both play a vital role in oral health and how one profession greatly influences the other. |
Instructor’s Guide
Background information. This simulation was pilot tested with a group of undergraduate speech-language pathology and audiology (SLPA) and dental students in years 1–3 of their program. This simulation is designed to help SLPA and dental students work together to understand the impact of common oral conditions on speech and speech development. Some of the exercises can be adapted for use with students of other health professions.
Overview for instructors. This simulation can be performed in any type of environment necessary (i.e., clinic, bedside, doctor’s office, or classroom). It allows SLPA and dental students to work together with the common goal of exchanging clinically relevant information so they may identify and implement appropriate care for patients suffering from common oral conditions.
As part of the simulation, three-dimensional tooth models representing various oral conditions were used, but if these are not available, photographs will suffice.
Materials provided in this toolkit.
- Case Scenario 1, Case Scenario 2, and Case Scenario 3 with complete information for instructors and for actors portraying patients.
- Handouts for students:
Additional materials.
- Three dimensional models (optional)
Instructor preparation.
- Recruit one to three trained actors to play the role of patient. The number of actors you recruit will depend on how many students you are training.
- Review the patient case scenarios with the standardized patients.
- Practice the simulation with the standardized patients prior to the actual simulation.
- Partner with dental faculty to recruit dental students who will work with the other students during the simulation to identify the oral condition and the course of action.
- Ask a faculty member from each of the programs participating in the simulation to locate or draft a short description of the roles and responsibilities for his or her profession. Compile these descriptions into one Word document and make it available to your students through email, your preferred learning management system, or your website.
- Refer to your roster and break students into groups of five or six before the day of the simulation. If possible, assign at least one dental student to each group.
Student preparation.
- Students should register for and complete the following Smiles for Life courses.
- Most SLPA students learn about oral mechanisms exams as part of their speech-language pathology criteria. However, if this is new information there is an abundance of online resources that can help to inform the student about this procedure.
- Students should review the roles and responsibilities document provided by the instructor prior to the simulation.
Schedule.
- Simulation orientation (5 minutes)
- Simulation (30 minutes)
Instructor’s Notes
This simulation will take each group of students approximately 35 minutes to complete.
Simulation orientation (5 minutes). Review learning objectives.
- Promote an in-depth understanding of how dentistry and speech-language pathology and audiology together contribute to oral health.
- Demonstrate how each of these professions influences the other.
Review the simulation process with the students.
- State the length of the simulation (35 minutes).
- Give each student a copy of Case Scenario 1.
- Explain the purpose of the three-dimensional models or photographs.
- Explain that students will break into pre-assigned teams and work together to complete the simulations.
- Note that groups should spend about 10 minutes on each patient case.
Simulation (30 minutes).
One standardized patient will work with each team to act out the three scenarios: (1) Acute dental injury that resulted in missing teeth, (2) ankyloglossia, and (3) tongue thrusting. A three-dimensional dental model or photographs representing the dental problem will accompany each scenario.
To conduct the simulation, teams should take the following steps.
- Enter the room as a team and interact with the standardized patient to determine what brought him or her into the office.
- Listen to the patient’s concerns, then examine the three-dimensional dental model or photographs together.
- Consider the patient’s history along with the clinical evidence found during the examination to assess the case.
- Document findings in real-time. Each team member should take his or her own notes.
- Consult with one another on findings and designate one team-member to report to the patient.
- Report findings to the patient and recommend a plan of treatment.
Case Scenario 1 (Instructor/Actor Copy)
You are a speech-language pathologist. A patient comes to you complaining of headaches and jaw pain.
Patient information.
Name: Tim
Age: 18
Occupation: Student
Reason for visit: Tim’s friends cannot understand him when he talks.
Background information. Tim has no other known medical complaints. Two weeks ago, Tim’s front wheel locked while he was riding his bike, throwing him over the handlebars. Tim landed face first on the pavement. He did not suffer any serious neck or back injuries.
Chief concern. When Tim fell off of his bike, he hit his mouth and is now missing three front teeth.
Dental consequences. Missing central incisors, as well as right lateral incisor. Loss of alveolar bone leading to collapse of lower facial 1/3 and mesial drift of right canine (#6) and left lateral incisor (#10).
Note: Dental faculty should be prepared to explain this terminology to the SPLA students.
Speech consequences. Reduced intelligibility. Tim has trouble correctly producing some phonemes. These include /s/, /θ/, /v/, and likely all alveolar sounds.
Note: SPLA faculty should be prepared to explain this terminology to the dental students.
Recommendations. An immediate consult and examination by a dentist is needed to address missing teeth and injury to surrounding tissues. The patient should also work with a speech-language pathologist to address speech development problems resulting from the accident.
Photographs. Top photographs are of three-dimensional models. The bottom photograph shows an actual clinical representation.

Photo: Emily Zimmerman, PhD, CCC-SLP, Assistant Professor, Department of Communication Sciences and Disorders, Bouvé College of Heath Sciences, Northeastern University.
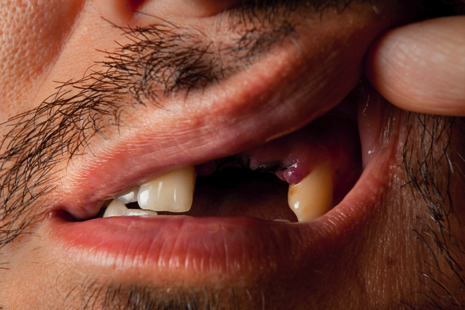
Photo: iStock.com/Ugur Atila
- What is the patient’s chief concern?
- What are the dental consequences of the patient’s oral condition?
- What are the speech consequences of the patient’s oral condition?
- What are your recommendations for this patient?
Case Scenario 2 (Instructor/Actor Copy)
You are a speech-language pathologist. A patient comes to you complaining of headaches and jaw pain.
Patient information.
Name: Michael
Age: 3
Occupation: Minor
Reason for visit: Michael’s mother cannot understand half of his speech.
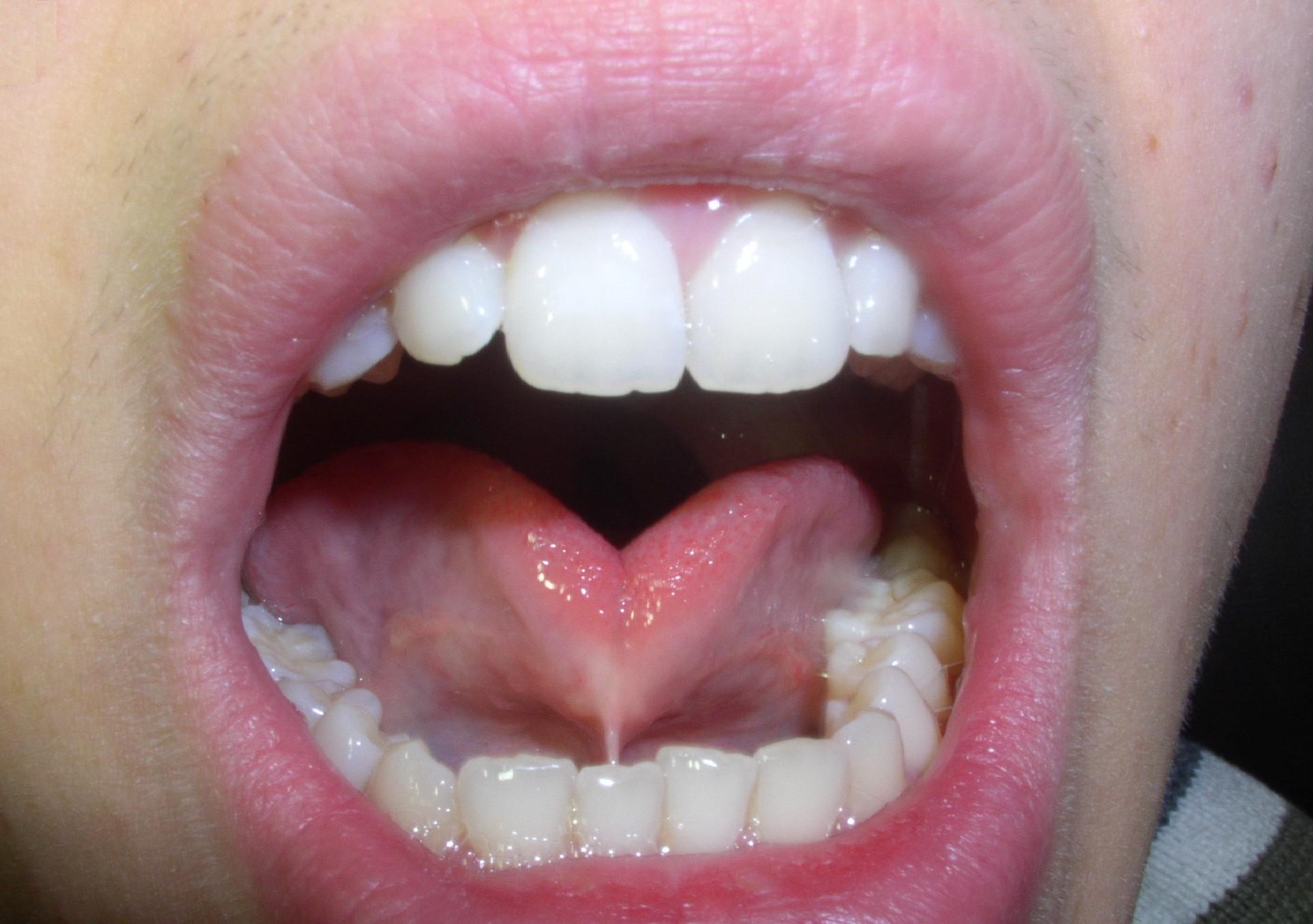
Background information. Michael was born with a short frenulum. His mother reports that she can only understand about half of what her son says. She also reports he had some difficulty sucking as an infant.
Chief concern. Michael has difficulty sucking, getting milk from a bottle, and licking, such as with an ice cream cone. It is also hard to understand him when he speaks.
Dental consequences. Ankyloglossia, lingual gingival recession, and diastema between mandibular central incisors (tooth numbers 25 and 26).
Note: Dental faculty should be prepared to explain this terminology to the SPLA students.
Speech consequences. Michael also has difficulty producing /t/, /d/, /n/, and /l/.
Overall health consequences. Michael has difficulty consuming certain foods.
Recommendations. Michael should be referred to a dentist to see if he is eligible to have his frenulum clipped. This would extend the length of his tongue and address his difficulties. If his speech problems do not resolve after his frenulum is clipped, Michael should work with a speech-language pathologist.
Photographs. Top photographs are of three-dimensional models. The bottom photograph shows an actual clinical representation.

Photo: Emily Zimmerman, PhD, CCC-SLP, Assistant Professor, Department of Communication Sciences and Disorders, Bouvé College of Heath Sciences, Northeastern University.
- What is the patient’s chief concern?
- What are the dental consequences of the patient’s oral condition?
- What are the speech consequences of the patient’s oral condition?
- What are your recommendations for this patient?
Case Scenario 3 (Instructor/Actor Copy)
You are a speech-language pathologist. A patient comes to you complaining of headaches and jaw pain.
Patient information.
Patient name: Sally
Age: 10
Occupation: Student
Reason for visit: Sally’s dentist will not apply braces until her tongue thrust is resolved.
Background information. Sally demonstrates a tongue thrust when she swallows. Her dentist says she needs braces, but her orthodontist will not put braces on until the tongue thrust is resolved. The orthodontist has explained that if the tongue thrust continues after the braces are removed, pressure from the tongue could move Sally’s teeth forward again.
Chief concern. Sally needs braces but can’t have them placed until she stops thrusting her tongue.
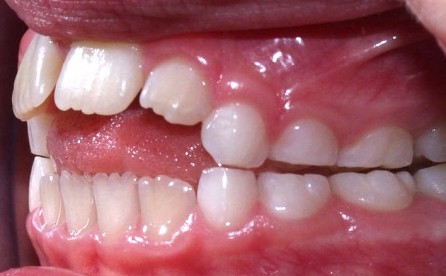
Dental consequences. Sally’s tongue thrust has pushed her top central incisors forward. This has caused an anterior open bite, protrusion, and rotation of the central incisors.
Note: Dental faculty should be prepared to explain this terminology to the SPLA students.
Speech consequences. Sally has difficulty producing /s/, /z/, “ch”, “sh”, and “zh.”
Recommendations. Sally’s dentist should refer her to a speech-language pathologist to address her tongue thrusting habit. The dentist and speech-language pathologist should collaborate to address this problem.
Photographs. Top photographs are of three-dimensional models. The bottom photograph shows an actual clinical representation.

Photo: Emily Zimmerman, PhD, CCC-SLP, Assistant Professor, Department of Communication Sciences and Disorders, Bouvé College of Heath Sciences, Northeastern University.
- What is the patient’s chief concern?
- What are the dental consequences of the patient’s oral condition?
- What are the speech consequences of the patient’s oral condition?
- What are your recommendations for this patient?
First Published: 11/2015
Last updated: 03/2016


