All healthcare professionals are driven, at least in part, by a desire to make a positive impact in the lives of their patients and the broader community.
Historically, this has been achieved through the prevention and treatment of injury and disease. As our understanding of health and wellness has evolved, however, we have come to realize that there is more to “health” than the physical factors we most often reference. In fact, where elements like nutrition, genetics, and exposure to infectious disease were previously considered the basis for “health” analysis, health professionals are now finding that there are a number of social factors that are just as impactful. These social factors are known as the social determinants of health (SDOH).
Read on to learn more about these critical factors and how trained professionals in the public health sector can address them in their work.
What Are The Social Determinants of Health?
The social determinants of health are the conditions in which we are born, live, work, play, and age, and which can affect a broad range of health outcomes including the likelihood of contracting a disease or of dying by a certain age. In public health contexts, these conditions are often referred to as the “places” that impact health.
Over the past three decades, the field of public health has experienced a dramatic shift toward a greater understanding and appreciation for the role of social determinants across a broad range of health outcomes. According to the Office of Disease Prevention and Health Promotion (ODPH), “health starts in our homes, schools, workplaces, neighborhoods, and communities. The conditions in which we live explain in part why some Americans are healthier than others, and why Americans more generally are not as healthy as they could be.”
Neil Maniar, professor of practice and director of the Master of Public Health program at Northeastern University has a similar outlook. “Where we live, work, learn, and play all have a profound influence on our health,” he says. “This idea is fundamental to the concept of social determinants of health.”
Download Our Free Guide to Preparing for a Career in Public Health
Learn more about how you can solve the complex problems facing complex environments.
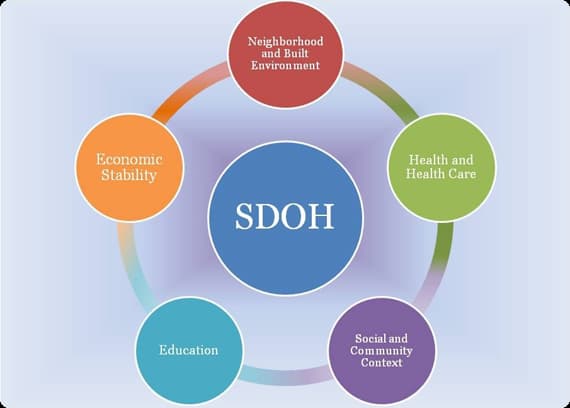
While there are many social determinants of health, the factors are commonly grouped into five main categories:
- Neighborhood: This area refers to the actual place in which an individual lives, and includes factors such as crime and violence rates, the quality of housing and infrastructure, access to ample and nutritious foods, and various other environmental considerations.
- Health and Healthcare: This area refers to various factors related to an individual’s health, which includes their level of health literacy, access to primary care and specialists, and access to healthcare in general.
- Social and Community Context: This area refers to factors related to an individual’s community and social support system, such as their level of civic participation, whether or not they face or have faced discrimination, whether they are or have ever been incarcerated, and the degree of social cohesion in their communities.
- Education: This area refers to both educational resources—including access to early childhood education and development, up-to-date textbooks and course materials, student-to-teacher ratios, etc.—and educational outcomes—including language skills and literacy, high school graduation rates, enrollment rates in higher education, etc.
- Economic Stability: This area refers to the various economic factors that may impact health outcomes, such as employment rates, poverty levels, food insecurity, housing instability, etc.
Social Determinants vs. Physical Determinants of Health
The social determinants of health are often discussed in relation to physical determinants of health—a concept which refers to the physical conditions of the environment in which a person lives. This is because the social and physical determinants of health are often woven together in ways that make it difficult to discuss either in pure isolation.
Still, the factors which fall under the categories of physical and social determinants of health vary greatly. Some of the most common examples of physical determinants of health include, but are not limited to:
- The natural environment: Weather and climate, climate change, soil and water quality, local plants, and wildlife
- The built environment: Buildings (homes, schools, recreational settings, etc.) and infrastructure (roads, walkways, bridges, etc.)
- Presence of contaminants: Toxic substances such as chemicals, mold, mildew, dust, dirt, pollen, and other detritus with the potential to do harm
- Physical barriers: Various constructs which may help or hinder access to certain resources. This factor is particularly important to the elderly, or individuals with disabilities. Some examples include walls, fences, curbs, stairs, elevators, ramps, and railings.
How Can Public Health Professionals Address Social Determinants of Health?
Although the social determinants of health are vast in scope, there are a number of evidence-based strategies that can effectively and sustainably mitigate their impact. We explore three of these top strategies below.
1. Raise awareness.
According to Maniar, one of the most effective ways of addressing the various social determinants of health is to raise awareness of those issues among both healthcare professionals and the general public.
For healthcare professionals, the benefits of this increased awareness and understanding is obvious: The more that doctors, nurses, administrators, and those that decide policy understand the impact of the social determinants of health, the better prepared they will be to understand patients, ask the right questions, and effectively communicate to patients about their health. Though they may appear small, these changes have the potential to ultimately improve overall health outcomes.
“Developing a greater understanding of the context within which health occurs can enable public health and healthcare professionals to more effectively improve the health of individuals, families, and communities,” Maniar says.
For members of the public, this understanding can encourage a more holistic view of one’s health, potentially leading individuals to ask more relevant questions of their healthcare providers and even make substantial lifestyle changes.
2. Consider short- and long-term effects.
For policymakers working to craft prevention programs and other policies that address various social determinants of health, it is critical that consideration is given both the immediate impact of an individual’s exposure to a condition and the potential long-term effects.
“Many of the determinants described above can not only impact health at multiple points across the lifespan but also lead to changes in health many years after the initial exposure,” Maniar says.
Real-World Example
Determinants such as education and family income have the potential to influence many different facets of health, as well. According to the 2012 National Survey of Children’s Health, over 30 percent of children in families who were below the federal poverty level reported poor health status, compared to less than seven percent of children in families who were at least 400 percent above the federal poverty level. The pathways that connect socioeconomic status to health can include access to care, health literacy, levels of social support, and exposure to environmental factors.
3. Advocate for policy changes that promote safe work and living conditions.
Whether within your own organization or at the government level (including local, state, regional, national, and international), advocating for and supporting policies that promote positive changes in public health can work to address determinants of social health in both direct and indirect ways.
Some examples of policies which may prove effective in this regard include, but are not limited to:
- Voucher programs: While many governments supply cash to citizens in need, research suggests that voucher programs may be more effective at promoting positive outcomes, such as facilitating access to healthcare or affordable nutrition.
- Educational support: Multiple studies conducted by the U.S. Department of Health and Human Services have shown that individuals who drop out of high school have increased odds of reporting various chronic health conditions, such as diabetes, hypertension, etc. One such report concludes that “policies and practices that reduce dropout may, in turn, impact the prevalence of chronic disease.” Similarly, it has been estimated that even just one year of college may decrease mortality rates from cancer and heart disease by 15-19 percent.
- Community development and housing programs: Recent studies have highlighted the role of neighborhood-level factors in shaping health outcomes. In many cases, these external factors were even more influential in driving health outcomes than one’s own genetic makeup. Studies of communities across the country have found that disparities across a range of health, social, and economic outcomes are concentrated within well-defined geographic boundaries. For example, the lower-income Boston neighborhoods of Roxbury, Dorchester, and Mattapan have consistently higher rates of cancer, cardiovascular disease, violence, and unemployment compared to more affluent neighborhoods such as Back Bay or Beacon Hill. Similar trends are observed in cities and towns throughout the country.
- Community health worker programs: Each neighborhood and community faces its own unique set of social-, economic-, and, ultimately, health-related challenges. Community health workers have the necessary skills and background needed to address these unique challenges, and the effectiveness of these programs has been demonstrated by multiple studies throughout the years.
Social Determinants and the Future of Public Health
The role of social determinants within the field of public health will continue to grow as our understanding of the various determinants and their impact continues to evolve.
“The integration of digital health, health informatics, and other rapidly developing technologies offer exciting opportunities to tackle social determinants and improve the health of individuals, families, and communities in innovative and long-lasting ways,” Maniar says. “Addressing social determinants of health also offer[s] public health professionals the opportunity to solve some of our most vexing public health problems, including the persistent disparities in health outcomes, the epidemic of violence, and the opioid epidemic.”
Individuals who are interested in addressing the social determinants of health can benefit from earning an advanced degree, he notes. Advanced public health degree programs give students the knowledge, skills, and frameworks to affect real and lasting change in their communities. The Master of Public Health (MPH) at Northeastern University, for example, was designed to help students examine how urban environments can affect a population’s wellbeing through the lens of the social determinants of health. It also explores ways graduates can use that understanding to communicate effectively with and advocate for diverse urban populations, both within the United States and abroad.
Learn more about the Master of Public Health at Northeastern on our program page, or download our free guide below to learn how to best prepare for a career in this vital industry.
This article was originally published in August 2018. It has since been updated for accuracy and relevance.







Related Articles
Jackney Prioly Joseph on How Her MPA Helped Her Career
Master’s in Nonprofit Management vs. Public Administration
How an MPH Clarified One Alumna’s Career Path